CENTRAL LINE ASSOCIATED BLOODSTREAM INFECTIONS IN NEONATAL AND PEDIATRIC UNITS IN GREECE
S. Kouni , C. Dimolitsa , E. Iosifidis , P. Kalabalikis , I. Kapetanakis , P. Karakosta , K. Katsibardi , M. Kazantzi , E. Kourkouni , P. Mexi , E. Nikaina , S. Papadopoulou , L. Petrikkos , T. Siahanidou , M. Skordala-Riti , A. Tragiannidis , M. Tsolia , K. Zannikos , TE. Zaoutis
36th Annual Meeting of the European Society for Paediatric Infectious Diseases (ESPID 2018)
Malmö, Sweeden, May 28- June 2, 2018
BACKGROUND: Healthcare-associated infections (HAI) are associated with increased morbidity and mortality and excess costs. Central line-associated bloodstream infections (CLABSI) are the most common HAI in neonates and children. The aim of this study was to develop a CLABSI collaborative network in neonatal and pediatric intensive care units and pediatric oncology units. Secondary objectives were to collect national benchmark data for CLABSI rates, isolated pathogens and antimicrobial susceptibility rates
METHODS: Active surveillance for CLABSI was conducted from June 2016 to February 2017. A collaborative network of 14 NICUs, 5 PICUs and 6 Pediatric Oncology Units (ONCs) participated in the program. Surveillance definitions of central line (CL), central line utilization (CLU) ratio, CLABSI event and CLABSI rate were based on 2014 Centers for Disease Control and Preventions’ National Healthcare Safety Network criteria. Medical records were assessed daily for calculating CL days, patient days and susceptibility of isolated organisms.
RESULTS: A total of 111 CLABSI episodes were recorded. The overall mean CLABSI rate was 4.41 infections per 1000 CL days and CLU ratio was 0.31. CLABSI rates were 6.02 in NICUs, 6.09 in PICUs and 2.78 per 1000 CL days in ONCs (Table). A total of 123 pathogens were isolated. The most common pathogens were Enterobacteriaceae (36%) followed by Gram-positive cocci (30%), non-fermenting Gram-negative bacteria (17%) and fungi (16%). Overall 38.5% and 37% of Gram-negative pathogens were resistant to third-generation cephalosporins and carbapenems, respectively.
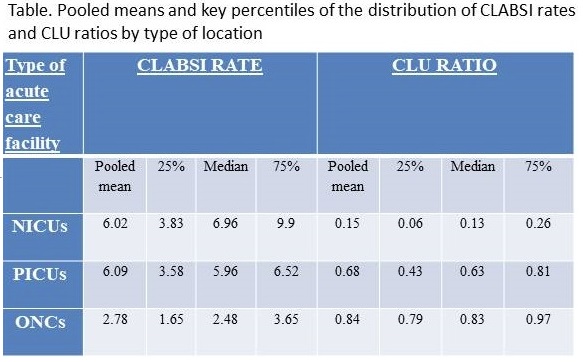
CONCLUSIONS: Nation-wide CLABSI rates were determined for pediatric patients. A worrying finding was the identification of high rates of carbapenem-resistant organisms. These data could be used to benchmark and serve as baseline data for the design and evaluation of infection control and antimicrobial stewardship interventions.



